 Consequently, some researchers are investigating risk score systems that identify patient-groups that can be discharged early with a low risk of harm from adverse cardiac events.įor an emergency physician, the short-term prognosis of a patient is paramount and therefore effectively defines the required accuracy of an investigative pathway. Considerable time and resources are consumed investigating the many patients who do not have an ACS. Despite prolonged workup, the actual number of patients finally diagnosed with ACS is often 25 % or less. Their safe workup generally requires considerable time and often includes in-patient observation, which adds to emergency-department and hospital overcrowding. Accordingly, assessment and safe disposition of these patients is a major challenge. Patients with symptoms suggestive of acute coronary syndromes (ACS) contribute approximately 5–10 % of annual presentations to emergency departments and up to 25 % of hospital admissions. Therefore, discharge decisions in emergency medicine are difficult to make and are frequently more challenging than treatment of an immediately life-threatening disease. If the numbers are significantly low, then adopting a risk-scoring system in an early rule-out strategy is unlikely to impact upon patient flow and emergency-department overcrowding.Ĭlinicians involved in acute care often worry that patients may come to harm, soon after discharge, from the medical complaint that they presented to the hospital with. Although sensitivity and negative predictive value are the key parameters of interest when deciding to use a risk-assessment score to assist with chest-pain rule-out decision-making, it is important to consider the proportion of patients that will be classified as low risk. The trend is towards systems using clinical logic and simple criteria. Scoring systems range from those developed from statistical weighting of variables collected in observational studies to those developed from clinical judgment, logic, and common sense. Consequently, researchers are increasingly modifying or developing cardiovascular risk-scoring systems for rule-out of acute coronary syndrome in patients who present to emergency departments with chest pain. TIMI risk can be calculated on the TIMI website under "Clinical Calculators.Considerable time and resources are consumed investigating the many patients who present to emergency departments but who do not have an acute coronary syndrome. 'TIMI risk' estimates mortality following acute coronary syndromes. 1 Pointĥ% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.Ĩ% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.ġ3% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.Ģ0% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.Ģ6% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization.Ĥ1% risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization. % risk at 14 days of: all-cause mortality, new or recurrent MI, or severe recurrent ischemia requiring urgent revascularization. *Risk factors include: family history of CAD, hypertension, hypercholesterolemia, diabetes, or being a current smoker. Severe angina (≥ 2 episodes w/in 24 hrs).Known coronary artery disease (CAD) (stenosis ≥ 50%).TIMI Score Calculation (1 point for each): In patients with UA/NSTEMI, the TIMI risk score is a prognostication scheme that categorizes a patient's risk of death and ischemic events and provides a basis for therapeutic decision making. Among the group's most important works is the TIMI Risk Score, which assesses the risk of death and ischemic events in patients with unstable angina (UA) or non-ST elevation myocardial infarction (NSTEMI). Braunwald held the chairmanship until 2010, when he appointed Marc Sabatine to the position. The TIMI Study Group was founded by physician Eugene Braunwald in 1984. 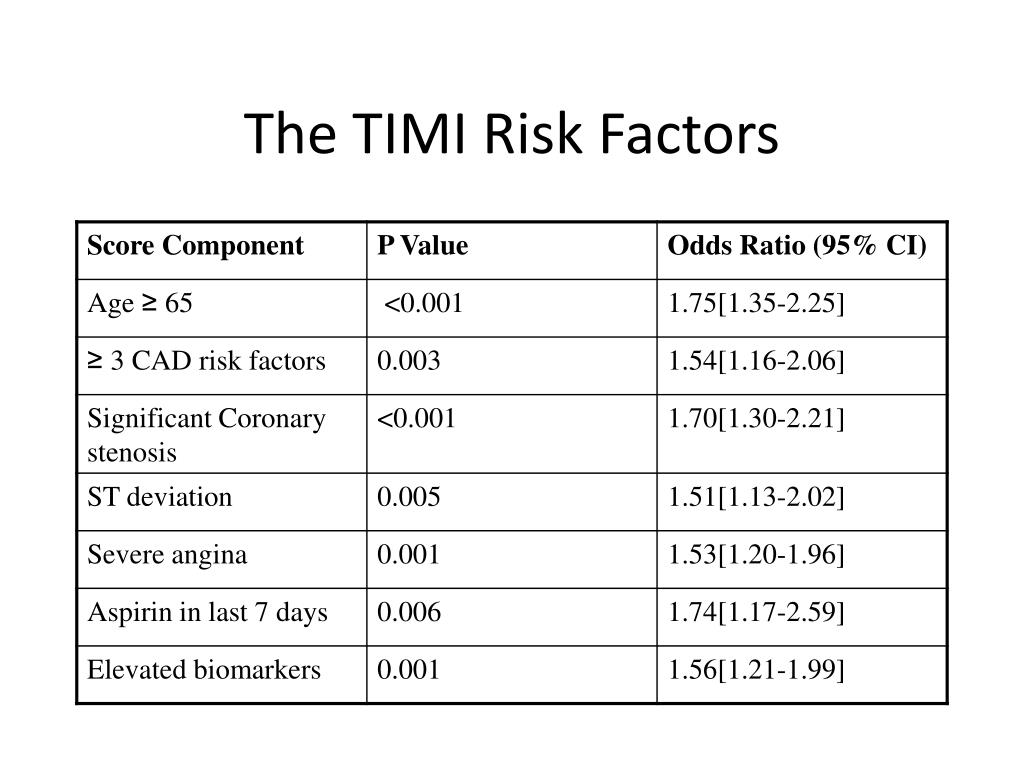
The group has its headquarters in Boston, Massachusetts. The Thrombolysis In Myocardial Infarction ( TIMI) Study Group, is an academic research organization (ARO) affiliated with Brigham and Women's Hospital and Harvard Medical School with a focus in the field of cardiovascular disease. For other uses, see Timi (disambiguation). For the IBM technology, see IBM i § TIMI. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
